Актуальность
Современный взгляд на гетерогенность трижды негативного рака молочной железы (ТНРМЖ) представляется скоординированной экосистемой, объединяющей «внутренние» подтипы ТНРМЖ и особенности микроокружения [1]. Хотя профилирование экспрессии генов является «золотым» стандартом для молекулярного субтипирования ТНРМЖ, целесообразность использования его в рутинной диагностике обсуждается, поскольку метод занимает много времени, дорог и требует свежезамороженной ткани. Кроме того, отсутствуют утвержденные критерии для определения подтипов ТНРМЖ с использованием морфологических, иммуногистохимических, генетических тестов или их комбинации, что ограничивает применение этих подтипов в клинических исследованиях и в повседневной практике.
В целом современное иммуногистохимическое исследование позволяет выделять четыре «суррогатных» подтипа рака молочной железы (РМЖ): люминальный А, люминальный В, HER2-позитивный и ТНРМЖ. В свою очередь ТНРМЖ является гетерогенным заболеванием. В различных исследованиях предпринимались попытки классифицировать ТНРМЖ на молекулярном уровне для выявления различных подтипов. Среди них в наиболее широко известных исследованиях изучали «внутренние» подтипы РМЖ PAM50 [2], подтип ТНРМЖ с низким уровнем клаудина [3] и подтипы ТНРМЖ, предложенные B.D. Lehmann et al. [4].
В соответствии с паттерном экспрессии генов «внутренние» подтипы по PAM50 классифицируют РМЖ на пять подтипов: люминальный A, люминальный B, HER2-обогащенный, нормальноподобный и базальноподобный. Этот метод относит большинство ТНРМЖ (47–88%) к базальноподобному типу [5].
Низкоклаудиновый подтип ТНРМЖ характеризуется низкой экспрессией люминальных маркеров дифференцировки и белков клеточных контактов, а также высокой экспрессией генов, связанных с эпителиально-мезенхимальным переходом и свойством стволовых клеток [3].
B.D. Lehmann et al. идентифицировали шесть подтипов ТНРМЖ (базальноподобный, 1-го и 2-го типов, иммуномодулирующий, мезенхимальный, мезенхимальный – стволоподобный и люминальный с экспрессией рецепторов андрогенов – LAR) [4]. Последующие исследования показали, что два из предложенных подтипов, а именно иммуномодулирующий и мезенхимальный (стволоподобный) не являются независимыми подтипами, а скорее обогащены большим числом инфильтрирующих опухоль лимфоцитов (TILs) или стромальных клеток соответственно [6].
M.D. Burstein et al. сообщили о 4 молекулярных подтипах, выявленных путем профилирования матричной РНК в 198 случаях ТНРМЖ: базальноподобном иммуносупрессивном (БИС); базальноподобном иммуноактивируемом (БИА), мезенхимальном и подтипе LAR [7]. Тип БИА показал гораздо более высокую стромальную лимфоцитарную инфильтрацию, чем тип БИС, что предполагает разницу в противоопухолевом иммунитете между двумя подтипами. Кроме того, БИС подтип ТНРМЖ был связан с худшими показателями безрецидивной выживаемости, чем другие типы [8].
Поскольку гетерогенность ТНРМЖ связана в т.ч. с опухолевым микроокружением, необходимы поиск и исследование более воспроизводимых биомаркеров, изучение их предиктивной и прогностической роли. Одним из таких биомаркеров в терапии РМЖ являются инфильтрирующие опухоль лимфоциты (TILs) – важные клетки адаптивной иммунной системы в микроокружении опухоли [9], подразделяющиеся на стромальные (sTILs) и внутриопухолевые (iTILs). Внутриопухолевые инфильтрирующие опухоль лимфоциты (iTILs) определяются как лимфоциты внутри кластеров опухолевых клеток, которые не взаимодействуют со стромой. Стромальные инфильтрирующие опухоль лимфоциты (sTILs) обнаруживаются в десмопластической строме между кластерами опухолевых клеток [10]. Исследования показывают, что sTILs – более воспроизводимый, чем iTILs, биомаркер и, как правило, хорошо коррелирует с iTILs [11].
TILs представляют собой популяцию клеток, состоящую из цитотоксических Т-лимфоцитов и Т-хелперов, а также В-лимфоцитов, макрофагов, естественных киллеров и дендритных клеток. Некоторые из этих клеток (цитотоксические Т-лимфоциты, T-хелперы1, макрофаги М1) обладают противоопухолевыми свойствами, а некоторые (В-лимфоциты, Т-хелперы2, макрофаги М2) обладают проопухолевыми свойствами [12, 13].
В результате воздействия цитостатических агентов развивается апоптоз или иммуногенная гибель клеток, высвобождение опухолевых неоантигенов приводят к усиленному поглощению дендритными клетками и последующей презентации антигена эффекторным Т-клеткам [14, 15]. Иммунологический ответ первоначально состоит из фазы элиминации с эффектом подавления опухолевого роста. В результате местной иммуносупрессии в микроокружении между опухолевыми клетками и иммунной системой развивается фаза равновесия и ускользания, наблюдается прогрессирование опухоли [16]. Этот процесс, называемый иммуноредактированием и обладающий противоопухолевыми и проопухолевыми свойствами, тесно связан с развитием и прогрессированием опухоли, а также считается одним из основных факторов, определяющих ответ на адъювантную и неоадъювантную терапию [17, 18]. Ранее РМЖ считался неиммуногенным заболеванием, теперь же на трижды негативный подтип РМЖ возлагаются большие надежды как на иммунологически зависимую опухоль, по крайне мере у части пациентов [19].
Поэтому оценка TILs в качестве биомаркера является важной задачей. Международная рабочая группа по иммуноонкологическим биомаркерам, также называемая «Рабочая группа TILs» (https://www.tilsinbreastcancer. org/pitfalls/), опубликовала руководство по повышению согласованности и воспроизводимости оценки TILs [20]. В руководстве подчеркивается, что стромальные TILs следует указывать в процентах. При этом с учетом потенциальной гетерогенности опухоли патологоанатомы должны оценивать различные области, а окончательный отчет должен отражать среднее значение.
Хотя подсчеты TILs стандартизированы [20, 21], данный показатель по-прежнему не влияет на стратегию лечения в международных и российских рекомендациях по лечению РМЖ [22, 23]. Почему такой простой и дешевый в определении биомаркер не вошел в рутинную практику?
Остаются проблемы, которые еще предстоит уточнить:
- какова степень влияния различных факторов на TILs;
- какова ассоциация TILs с прогнозом в реальной практике;
- какова воспроизводимость TILs между патологами;
- какие существуют проблемы и ограничения правил по определению TILs в реальной практике;
- нет представления об общепринятой границе между высоким и низким уровнями TILs в клинической практике;
- недостаточно данных для принятия решений по лечению на основе уровня TILs.
Предиктивная и прогностическая роль TILs в проводимых исследованиях
Высокий уровень TILs определяется примерно в 20% случаев ТНРМЖ [24]. Во многих крупных клинических исследованиях повышенный уровень TILs в микроокружении опухоли у больных ранним ТНРМЖ ассоциируется с улучшением показателей безрецидивной выживаемости (БРВ), общей выживаемости (ОВ) и частоты полного патоморфологического ответа (pCR) [25–28]. Корреляция между высоким уровнем TILs в опухолевой ткани до лечения и более высокими показателями pCR наблюдалась в ряде неоадъювантных исследований (см. таблицу). В основополагающих исследованиях GeparDuo и GeparTrio (высокий уровень TILs коррелировал с более высоким показателем pCR) частота pCR у больных РМЖ с преобладанием TILs составила 43 и 52% соответственно [29]. В исследовании GeparSixto, в котором сравнивали платиновую и бесплатиновую неоадъювантную химиотерапию (НАХТ), у 28% пациентов в подгруппе ТНРМЖ отмечен фенотип с преобладанием стромальных лимфоцитов. У пациентов данной подгруппы наблюдалась очень высокая частота достижения pCR (74%) при лечении НАХТ с включением антрациклиновых антибиотиков, таксанов и препаратов платины [30]. Интересно, что абсолютная частота достижения pCR при ТНРМЖ с преобладанием лимфоцитов была намного выше при лечении режимами на основе препаратов платины по сравнению с бесплатиновыми режимами (74 против 43%). Эти данные свидетельствуют, что НАХТ на основе карбоплатина может быть опцией выбора в лечении больных ТНРМЖ с высоким содержанием TILs. Аналогично в исследовании BrighTNess [31] показано, что у больных с более высокой инфильтрацией CD8+-T-лимфоцитов в опухоли отмечены лучшие результаты от карбоплатинсодержащей НАХТ. В двойном слепом плацебо-контролируемом исследовании GeparNuevo (II фазы) пациенты с ранним ТНРМЖ (n=174) были рандомизированы для получения дурвалумаба в сочетании со стандартной НАХТ (sTILs оценивался в качестве биомаркера для стратификации пациентов во время рандомизации) [32]. Результаты по частоте pCR были статистически незначимы в группе иммунотерапии (ИТ) по сравнению с группой плацебо – 53,4 и 44,2% соответственно (p=0,224). Однако у пациентов с более высокими TILs в обеих группах исследования значительно улучшилась частота достижения pCR (p<0,01), хотя сами TILs не были конкретно связаны с ответом на дурвалумаб. Недавний анализ этого исследования показал, что TILs были независимым предиктором pCR [33].
В немецком исследовании NIB (II фазы) пациенты получают неоадъювантную терапию пембролизумабом в сочетании с наб-паклитакселом, эпирубицином и циклофосфамидом с ранним ТНРМЖ. Дополнительно исследуются уровень sTILs на исходном уровне в дополнение к другим потенциальным биомаркерам, таким как мутационная нагрузка и микробиота.
Недавно опубликованные результаты исследований IMpassion-031 [34], KEYNOTE-522 [35] и I-SPY2 [36] не выявили зависимости эффективности ИТ от уровня PD-L1, что подчеркивает необходимость изучения других биомаркеров для прогнозирования исходов для пациентов с ТНРМЖ, получавших НАХТ в комбинации с ингибиторами точек иммунного контроля.
В неоадъювантном исследовании KEYNOTE-522 (III фазы) оценивалась целесообразность добавления пембролизумаба к НАХТ у пациентов с ТНРМЖ [35]. В общей сложности 602 пациента получали пембролизумаб в комбинации с НАХТ (паклитаксел и карбоплатин, далее доксорубицин/ эпирубицин и циклофосфамид) или плацебо плюс НАХТ в соотношении 2:1. Промежуточный анализ показал, что пациентами, получавшими НАХТ на основе пембролизумаба, достигнута более высокая частота pCR по сравнению с группой плацебо (64,8 против 51,2%; p<0,001) независимо от статуса PD-L1. Точно так же показатели 18-месячной БСВ были достоверно выше при адъювантной терапии, содержавшей пембролизумаб (91,3 против 85,3%; р<0,001) [35].
В отличие от этих результатов в исследование III фазы NeoTRIP были включены 280 пациентов с ранней стадией ТНРМЖ, получавших НАХТ на основе карбоплатина и набпаклитаксела с ИТ атезолизумабом или без него с целью оценки 5-летней бессобытийной выживаемости (БСВ) [37]. По последним представленным результатам, частота pCR была ненамного численно выше в группе атезолизумаба (43,5 против 40,8%); результаты 5-летней БСВ ожидаются.
По-прежнему остается неясным:
- каким пациентам необходимо добавление ИТ при раннем ТНРМЖ высокого риска (cT2N1, cT3N0-1);
- какой режим НАХТ в комбинации с ИТ оптимальный;
- требует уточнения баланс эффективности и рисков токсичности от назначенной терапии;
- как оптимизировать подход к лечению раннего ТНРМЖ, пытаясь при этом максимально индивидуализировать его?
В перспективе привлекателен подход к возможному отказу от химиотерапии пациенток низкого риска. В одном из таких исследований при анализе пациенток младше 40 лет с клинически негативными лимфатическими узлами, которые не получали неои адъювантной химиотерапии, и с высоким уровнем TILs (≥75%), 15-летняя кумулятивная частота развития отдаленных метастазов или летального исхода составила всего 2,1% случаев, тогда как у пациенток с низким уровнем TILs (<30%) 15-летняя кумулятивная частота отдаленного метастазирования или летальных исходов составила 38,4% случаев. Кроме того, доказано, что каждые 10% прироста TILs были ассоциированы со снижением риска летального исхода на 19% [38].
Уровень TILs не только изучался как предиктор ответа на НАХТ, но и оценивалась его прогностическая роль в резидуальной (остаточной) опухоли. Показано, что высокие уровни TILs в резидуальной опухоли после НАХТ связаны с показателями лучшей БРВ и ОВ [39, 40]. Оцененные в резидуальной опухоли TILs совместно с оценкой RCB (остаточная опухолевая нагрузка) также являются важным предиктором рецидива заболевания после НАХТ и могут быть более чувствительными показателями, чем только TILs без патоморфологического изучения RCB [41].
С учетом связи высоких значений TILs с улучшением долгосрочных исходов при раннем ТНРМЖ будущие исследования эффективности нео/ адъювантного лечения должны предусматривать определение TILs для возможной деэскалации режимов химиотерапии. Основываясь на многообещающих прогностических данных, экспертная группа St Gallen International Consensus, 2019 и 2021, рекомендует рутинно определять TILs при ТНРМЖ, однако данных по-прежнему недостаточно, чтобы рекомендовать TILs в качестве биомаркера для выбора нео/адъювантного лечения [42, 43]. Пятое издание классификации опухолей ВОЗ (опухоли молочной железы) также подтвердило целесообразность гистопатоморфологической количественной оценки TILs при ТНРМЖ и HER2-позитивных РМЖ, выраженной как среднее процентное содержание лимфоплазмоцитарной инфильтрации стромы опухоли [44].
Заключение
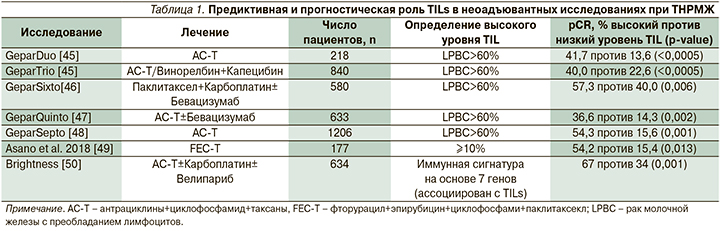
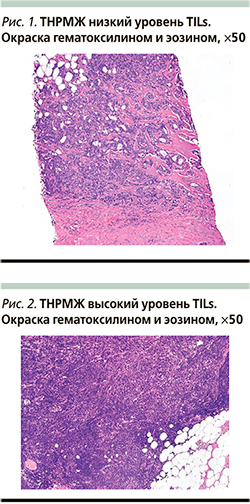
Инфильтрирующие опухоль лимфоциты (TILs) – это недорогой надежный прогностический и предиктивный биомаркер, который представляет собой «суррогат» противоопухолевого Т-клеточного иммунитета. Однако отсутствуют доказательства того, что решение о лечении, основанные на TILs, всегда благоприятно влияют на исходы пациентов. Тем не менее TILs можно использовать пациентам с хорошим прогнозом для изучения подходов к деэскалации лечения и тем самым снижения токсичности. Больным трижды негативным раком молочной железы TILs должны быть включены в качестве биомаркеров при проведении клинических испытаний. Поскольку для оценки TILs необходимы простые инструменты, такие как микроскоп и простая окраска «гематоксилин-эозин» (рис. 1, 2), – все это создает возможности для проверки «клинической пользы» TILs и для внедрения оценки такого маркера, как инфильтрирующие опухоль лимфоциты, в рутинную клиническую практику.
Вклад авторов. Т.Ю. Семиглазова – обзор публикаций по теме статьи, научное редактирование рукописи. А.С. Артемьева, А.Г. Кудайбергенова, С.М. Шарашенидзе, А.И. Целуйко, Р.М. Палтуев, В.В. Семиглазов, П.В. Криворотько, В.Ф. Семиглазов – научное редактирование рукописи. Ш.Р. Абдуллаева – написание текста рукописи, обзор публикаций по теме статьи.
Финансирование. Работа проведена без спонсорской поддержки.



