Обоснование
Значимость коморбидных инфекций (КИ) при ревматических заболеваниях (РЗ) определяется их влиянием на активность, характер проводимой терапии и прогноз из-за присутствующей иммуносупрессии [1, 2]. Причиной вторичного иммунодефицита является как сама ревматологическая патология, так и в применение цитостатиков, глюкокортикостероидов (ГКС), а в последнее время – активное использование генно-инженерных биологических препаратов (ГИБП) [3]. Выраженность иммуносупрессии подчеркивает нарастающая частота пневмоцистоза у пациентов ревматологического профиля [4]. Немаловажным дополнением является и эпидемиологическая обстановка, обусловившая высокую частоту применения ГКС, ГИБП и антимикробных средств в популяции в целом. Среди РЗ, требующих иммуносупрессивной терапии, наиболее часто встречается ревматоидный артрит (РА): в возрасте 35–55 лет данная патология регистрируется у 0,5–1% населения, в гериатрических группах число пациентов достигает 2% [5].
Цель исследования: оценка частоты, нозологической структуры и факторов риска КИ при РЗ у пациентов ревматологического отделения ГБУЗ «Республиканская больница им. В.А. Баранова», Петрозаводск.
Методы
Проведен ретроспективный анализ всех историй болезни пациентов, находившихся на стационарном лечении в ревматологическом отделении ГБУЗ «Республиканская больница им. В.А. Баранова» (Петрозаводск) в 2018–2022 гг. КИ диагностировали на основании клинической картины в сочетании с лабораторно-инструментальными данными в соответствии с действующими клиническими рекомендациями Минздрава РФ и рекомендациями профессиональных сообществ [6–14].
В ревматологическое отделение ГБУЗ «Республиканская больница им. В.А. Баранова» (Петрозаводск) госпитализируются пациенты только ревматологического профиля, проживающие в Республики Карелия и имеющие показания к госпитализации.
Анализировали истории болезни за 5 лет с целью регистрации КИ. Ввиду преобладания КИ среди пациентов с РА более детально проанализирована данная категория больных. Диагноз РА устанавливался согласно критериям ACR/EULAR-2010 [15]. Пациенты были разделены на две группы в зависимости от вида проводимой базисной противовоспалительной терапии: получавшие ГИБП и получавшие традиционные базисные противовоспалительные препараты (БПВП). Для уточнения факторов риска КИ более детально проанализированы истории болезни пациентов с РА, находившихся на стационарном лечении в ревматологическом отделении ГБУЗ «Республиканская больница им. В.А. Баранова» в 2020 г. Учитывали все бактериальные и вирусные инфекции, соответствовавшие установленным критериям диагностики [6–14].
Протокол исследования рассмотрен на заседании Этического комитета ГБУЗ РК «Республиканская больница им. В.А. Баранова» 01.02.2023 (протокол № 160). Постановление комитета: «Одобрить проведение исследования, проводимого кафедрой госпитальной терапии ФГБОУ ВО «Петрозаводский государственный университет» на базе ревматологического отделения ГБУЗ РК «Республиканская больница им. В.А. Баранова» «Коморбидные инфекции в ревматологии: ретроспективный анализ (по данным ГБУЗ «Республиканская больница им. В.А. Баранова», Петро-заводск, Республика Карелия)».
Размер выборки предварительно не рассчитывался. Статистическая обработка полученных результатов проводилась с использованием пакета статистического анализа данных Statistica 13.3, включая описательную статистику, корреляционный анализ по методу Спирмена, χ2-критерий (точный критерий Фишера с учетом небольшого числа «исходов») и отношение шансов (ОШ). Различия считали статистически значимыми при p<0,05.
Результаты
Проанализировано 8362 истории болезни пациентов с РЗ. Общее число историй болезни за изучаемые годы и истории болезни госпитализированных по поводу РА представлены на рис. 1.
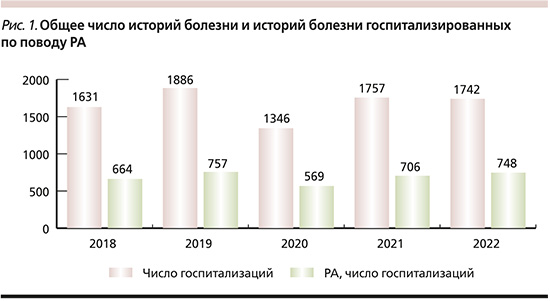
На рис. 2 – число пациентов, лечившихся в отделении по поводу РА в 2018–2022 гг., и число больных РА, получавших ГИБП.
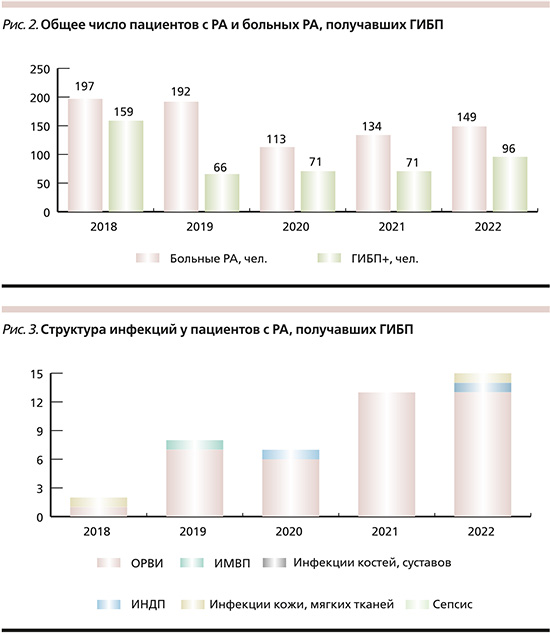
Число историй болезни, пациентов и КИ при отдельных РЗ отражено в табл. 1.
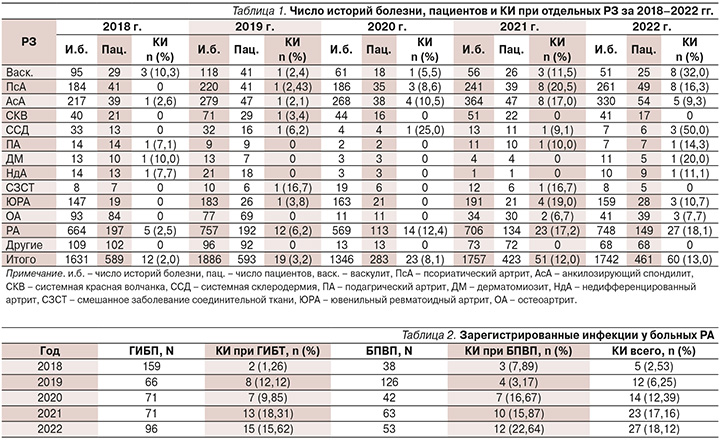
Число КИ при РА составило 49,09% от общего числа КИ при всех РЗ, в связи с чем дальнейший анализ проводился только в отношении пациентов с РА.
Частота КИ при РА в зависимости от проводимой базисной терапии указана в табл. 2.
При анализе нозологических форм КИ при РА обращало на себя внимание различие в их структуре при сравнении групп пациентов, получавших ГИБП и традиционные БПВП. Так, в группе пациентов с РА, получавших ГИБП, во все годы преобладали вирусные инфекции респираторного тракта. Структура инфекций у пациентов с РА, получавших ГИБП и другие БПВП, приведена на рис. 3, 4.

При изучении различий между группой пациентов, получавших ГИБП, и группой на базисной терапии другими препаратами достоверных различий не получено (p>0,05), что свидетельствует об отсутствии разницы в частоте развития инфекций в анализируемых группах (терапия ГИБП не увеличивает риска развития КИ) (табл. 3).
Ввиду большого числа вирусных инфекций легкого течения вторично проанализированы исключительно инфекции, имевшие клиническое значение (потребовавшие отмены базисной терапии и госпитализации). Получены результаты, свидетельствовавшие о большей частоте инфекций в группе пациентов, получавших традиционные БПВП (во все годы ОШ менее единицы, но достоверные различия, согласно ДИ, получены только в 2018 и 2020 гг., при этом в 2020 г. различия достоверны и при оценке χ2-критерия (р=0,010), табл. 4).

Для уточнения факторов риска КИ более детально проанализированы истории болезни пациентов с РА, находившихся на стационарном лечении в ревматологическом отделении ГБУЗ «Республиканская больница им. В.А. Баранова» в 2020 г. Всего за данный год госпитализированы 119 пациентов с РА (88 женщин, 31 мужчина, средний возраст – 57,803±12,09 года) с числом госпитализаций в течение года от 1 до 13. Диагноз РА устанавливался согласно критериям ACR/EULAR-2010. Средняя длительность РА составила 12,60±7,91 года. В проанализированной группе пациентов инфекции выявлены у 14 человек, из них 6 случаев бактериальной инфекции (2 – костей и суставов, 2 – нижних дыхательных путей, 1 – сепсис, 1 – мочевыводящих путей), у остальных больных регистрировалась коронавирусная инфекция COVID-19 разной степени тяжести. В качестве базисной терапии 75 человек получали ГИБП, 51 (68%) из них в сочетании с метотрексатом. В качестве базисного противовоспалительного препарата в группе пациентов, не получавших ГИБП, также преобладал метотрексат – 25 (55,5%) человек. При изучении корреляции отдельных характеристик пациентов с развитием КИ получены данные, представленные в табл. 5. Так, статистически значимой оказалась связь между развитием КИ и активностью РА, а также терапией ГКС в дозе более 7,5 мг/сут. по преднизолону.
Обсуждение
Среди пациентов, госпитализированных в ревматологическое отделение ГБУЗ «Республиканская больница им. В.А. Баранова» за 5 лет, преобладали больные РА. В той же группе пациентов выявлено наибольшее число КИ. Структура КИ имела различия в зависимости от вида базисной противовоспалительной терапии. Различия в частоте КИ в подгруппах пациентов, получавших ГИБП и традиционные БПВП, статистически не достоверны во все проанализированные годы. Статистически значимой явилась связь между развитием КИ и активностью РА, а также терапией ГКС в дозе 7,5 мг/сут и более по преднизолону.
РА – одно из наиболее частых иммуновоспалительных заболеваний в ревматологии [5], при котором инфекции развиваются в 1,5–2,0 раза чаще по сравнению с популяцией [1, 3]. В последние годы значимо возросла частота использования ГИБП и ГКС как по поводу самого РА, так и ввиду эпидемиологической обстановки. Применение ГКС повышает риск бактериальных инфекций [16]; полученные результаты в проведенном нами исследовании соответствуют данному утверждению. Корреляция КИ с активностью РА, наиболее вероятно, объясняется как более агрессивной иммуносупрессивной терапией, назначаемой при высокой активности заболевания, так и повышением острофазовых показателей в ответ на развитие КИ. Согласно литературным данным, к значимым факторам риска КИ при РА относятся хронические болезни почек и легких, сердечно-сосудистая недостаточность и сахарный диабет [1]. В нашем исследовании данные факторы не анализировались ввиду небольшого размера выборки.
Несмотря на большой объем проанализированной информации, результаты проведенного исследования следует трактовать с осторожностью по причине ретроспективного характера исследования, ограниченного числа госпитализаций ввиду эпидемиологической обстановки и недостаточной статистической мощности вследствие небольшого объема выборки пациентов с КИ.
Заключение
КИ при иммуновоспалительных заболеваниях осложняют течение основной патологии, нередко требуют отмены базисной противовоспалительной терапии, таким образом негативно влияя на прогноз, качество жизни, повышают смертность. Нозологическая структура инфекций разнородна, зависит от характера иммуновоспалительного заболевания, сопутствующей патологии. Своевременная диагностика инфекций затруднительна ввиду зачастую стертой клинической картины, что обусловлено проводимой базисной противовоспалительной иммуносупрессивной терапией. Сочетание сложности диагностики, наличия иммуносупрессии и растущей по разным причинам антибиотикорезистентности значимо осложняет качественное лечение пациентов, требуя разработки стандартов обследования больных ревматологического профиля, выделения факторов риска развития КИ при различных иммуновоспалительных заболеваниях. Проведенное нами исследование вновь обозначило наиболее весомую когорту пациентов с РА с точки зрения частоты развития КИ. Получена информация о различии в структуре КИ в зависимости от вида базисной терапии. Выделены наиболее часто сочетающиеся с развитием КИ такие факторы риска, как высокая активность РА и применение ГКС в дозе 7,5 мг/сут и более по преднизолону. Полученные результаты помогут обозначить группу больных РА, требующих особого внимания и дообследования на предмет КИ в случае повышения активности основного заболевания. Перспективными вариантами решения данной проблемы являются своевременная вакцинация (пневмококковая вакцина, вакцинация от новой коронавирусной инфекции, вируса гриппа), рациональное назначение антимикробных препаратов и ГКС, поиск новых лабораторных методов, которые позволят достоверно своевременно верифицировать развитие КИ, проводить дифференциальный диагноз с обострением основного заболевания.
Вклад авторов. И.М. Марусенко – концепция и дизайн исследования. Н.Д. Сильвестрова, Я.А. Авдеева – сбор и обработка материала. Н.Л. Рябкова – статистическая обработка данных, написание текста. В.А. Рябков – редактирование.



