Антиконвульсанты широко применяют в неврологической и психиатрической практике для лечения эпилепсии, аффективных расстройств и хронических болевых синдромов. Одним из наиболее хорошо изученных препаратов этой группы является ламотриджин, потребление которого продолжает расти во всех странах мира, особенно при биполярном аффективном расстройстве (БАР) [1–3].
Ламотриджин обладает множественными механизмами действия, которые лежат в основе его разнообразных фармакологических эффектов, в т.ч. не характерных для других антиконвульсантов. Основным механизмом действия ламотриджина считается блокада вольтажзависимых натриевых каналов, приводящая к угнетению выброса в синоптическую щель возбуждающих аминокислот, таких как глутамат и аспартат [4, 5]. Другие механизмы действия препарата включают блокаду потенциалзависимых кальциевых каналов, приводящую к снижению гиперактивности нейронов в зоне СА1 гиппокампа, отвечающей за регуляцию эмоциональной сферы и когнитивные функции [6]. При длительном применении он также повышает содержание в головном мозге тормозного медиатора γ-аминомасляной кислоты (ГАМК) [4, 5]. Ламотриджин способен угнетать моноаминоксидазу (МАО) [7], угнетать обратный нейрональный захват серотонина, норадреналина и дофамина и стимулировать серотонинергическую передачу [8], что, по-видимому, лежит в основе его антидепрессивного действия. Нейропротективное действие ламотриджина и терапевтический эффект при БАР могут быть связанными с его глутаматергической активностью [9]. Возможно, что ламотриджин имеет и другие пока неизвестные механизмы действия, которые объясняют его эффективность при БАР [10].
Эффективность ламотриджина при биполярном аффективном расстройстве Лечение БАР включает три этапа терапии:
- купирующую;
- поддерживающую (долечивающую);
- профилактичеcкую (противорецидивную) [11].
При остром эпизоде мании во всех международных и отечественных рекомендациях в качестве препаратов выбора рассматриваются нормотимики. Однако антиманиакальный эффект не является классовым эффектом препаратов этой группы и характерен только для лития, карбамазепина и вальпроата [12]. Ламотриджин в виде монотерапии изучался у пациентов с острой манией в пяти предрегистрационных исследованиях и ни в одном из них не превосходил по эффективности плацебо [13].
В отличие от острого эпизода мании единое мнение экспертов в отношении препаратов выбора при остром эпизоде депрессии отсутствует, что находит отражение в рекомендациях разных стран [14]. Ламотриджин относится к числу наиболее хорошо изученных препаратов при данном состоянии, поэтому в виде монотерапии или в комбинации с другими препаратами рассматривается в качестве терапии первой линии во всех международных и национальных рекомендациях [14]. Среди антиконвульсантов кроме ламотриджина имеющиеся доказательные данные позволяют рекомендовать в качестве препарата первого выбора при депрессивном эпизоде только вальпроат [15], однако его применение многими категориями пациентов, прежде всего беременными женщинами и женщинами детородного возраста, в целом ограничивают побочные эффекты, включая тератогенный, и повышенный риск развития синдрома поликистозных яичников [16–18].

Эффективность ламотриджина при остром эпизоде депрессии изучалась в предрегистрационном периоде в пяти рандомизированных клинических исследованиях (РКИ) продолжительностью 7–10 недель [19]. Их мета-анализ показал, что ответ на лечение ламотриджином наблюдался у существенно большего числа пациентов в группе ламотриджина, чем в группе плацебо, при оценке по шкале как Гамильтона (HAM-D – Hamilton Depression Rating Scale), так и Монтгомери-Асберг (MADRS – Montgomery-Asberg Depression Rating Scale). Однако в регрессионном мета-анализе было выявлено, что препарат эффективен только в отношении больных тяжелой (>24 баллов по шкале HAM-D), но не легкой депрессией [20]. Результаты еще одного анализа объединенных данных этих исследований, в котором оценивались пункты шкалы HAM-D, ассоциированные с улучшением при применении ламотриджина, позволяют предположить, что его клиническая польза при остром эпизоде биполярной депресии преимущественно связана с устранением депрессивного настроения (начиная с 3-й недели) и психомоторной заторможенности (начиная с 4-й недели) [21].
В пострегистрационном периоде антидепрессивная активность ламотриджина была продемонстрирована в многоцентровом двойном слепом плацебо-контролируемом РКИ с участием 195 пациентов с умеренной депрессией в рамках БАР I [22]. Она подтвердилась и в крупном многоцентровом двойном слепом плацебо-контролируемом исследовании, включившем 200 пациентов с БАР I и БАР II [23].
В этом исследовании препарат по эффективности превосходил плацебо во всех изученных дозах (100–400 мг/сут) и был более эффективным для пациентов с БАР I, чем с БАР II. Согласно результатам систематического обзора 21 РКИ, в котором оценивалась эффективность разных препаратов при остром эпизоде депрессии при БАР II, ламотриджин может рассматриваться для этих пациентов как препарат со «смешанной» поддержкой (с противоречивыми доказательными данными) [24].
По эффективности при остром эпизоде депресии при БАР I ламотриджин уступает кветиапину и немного – комбинации оланзапина с флуоксетином, но превосходит их по переносимости [25, 26].
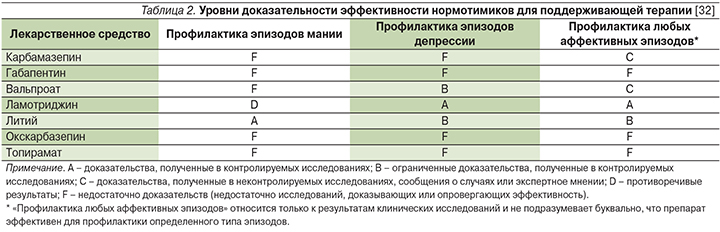
Уровень доказательности эффективности ламотриджина при остром эпизоде депрессии рассматривается как наивысший («А») (табл. 1). Это послужило основанием для включения ламотриджина в качестве препарата первого выбора при остром эпизоде биполярной депрессии во многие рекомендации, включая совместные Международного общества биполярных расстройств (ISBD – International Society for Bipolar Disorders) и Канадской сети по лечению расстройств настроения и тревоги (CANMAT – Canadian Network for Mood and Anxiety Treatments), рекомендации Международной консенсусной группы по доказательной фармакотерапии депрессии при БАР I и БАР II (ICG – International Consensus Group on the Evidence-based Pharmacologic Treatment of Bipolar I and II Depression), а также ряд национальных рекомендаций [14]. Тем не менее полный консенсус экспертов по данному вопросу отсутствует, т.к. применение монотерапии препаратом в острых ситуациях может ограничивать необходимость медленной (в течение 6 недель) титрации его доз с целью предотвращения развития серьезной сыпи [27, 28]. Возможно применение комбинации ламотриджина с литием, которая, по мнению экспертов Всемирной психиатрической ассоциации, наиболее эффективны в данной клинической ситуации [18].
В некоторых руководствах по лечению БАР ламотриджину рекомендуется отдавать предпочтение в отношении пациентов со смешанными эпизодами (наличие симптомов депрессии во время эпизода гипомании или симптомов гипомании во время эпизода депрессии) [29] и с быстрой цикличностью (не менее четырех аффективных эпизодов в год ) в случае преобладания у них депрессивной симптоматики [30].
Доказательства высокого уровня подтверждают применение ламотриджина для длительной поддерживающей терапии БАР (табл. 2). В трех плацебо-контролируемых исследованиях применение ламотриджина в суточных дозах 50–400 мг позволило существенно пролонгировать время до развития любого аффективного эпизода у пациентов с БАР I, недавно перенесших эпизод мании или гипомании [18]. Обобщенный анализ результатов двух исследований показал, что в течение 18 месяцев ламотриджин снижал риск развития аффективного эпизода любой полярности на 36%, однако был более эффективным в отношении профилактики рецидивов депрессии, чем мании [31].
Эффективность профилактического применения ламотриджина больными БАР I подтверждена результатами мета-анализов [33, 34]. Она повышается при его применении в составе комбинированной терапии, однако последняя ассоциируется с более высоким риском развития побочных эффектов. [18]. В то же время монотерапия ламотриджином имеет преимущества перед большинством других препаратов при длительном применении с точки зрения переносимости [35].
Во всех современных руководствах по лечению БАР ламотриджин рассматривается в качестве препарата первой линии для поддерживающей терапии БАР, однако в большинстве из них оговаривается, будто он показан пациентам с преобладанием депрессии [14]. Роль ламотриджина в профилактике эпизодов мании требует дальнейшего изучения.
Безопасность ламотриджина
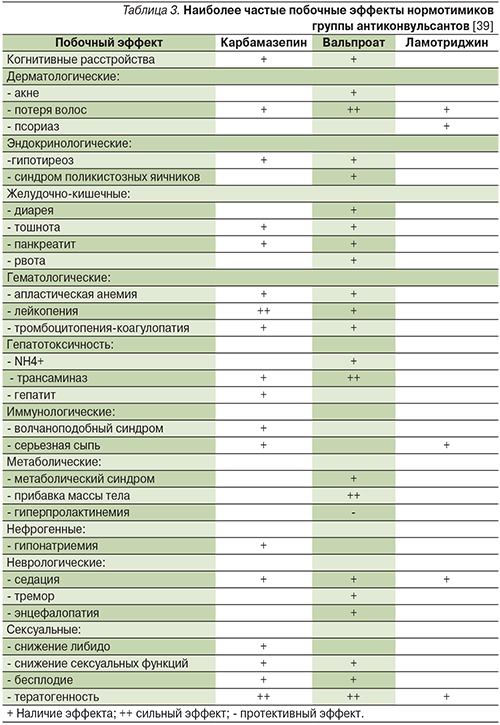
Ламотриджин обладает значительно более благоприятным профилем побочных эффектов по сравнению с другими антиконвульсантами, применяемыми для лечения БАР (табл. 3). При применении в суточной дозе 100–200 мг он отличается прекрасной переносимостью, а убедительные данные о повышении эффективности препарата больными БАР в дозах выше 200 мг/сут отсутствуют [13].
В клинических исследованиях, в т.ч. продолжительностью 18 месяцев, частота отмены из-за побочных эффектов не различалась в группах ламотриджина и плацебо [36, 37]. Наиболее частым побочным эффектом ламотриджина в РКИ была головная боль, однако достоверно чаще, чем в группе плацебо, она встречалась лишь в одном исследовании [9]. Головная боль, а также другие относительно частые побочные эффекты, такие как головокружение и тошнота, наиболее часто развиваются при одновременном применении с вальпроатом [38].
Ламотриджин может вызывать гематологические нарушения (нейтропению, лейкопению, анемию, тромбоцитопению, панцитопению, апластическую анемию, агранулоцитоз) и нарушение функции печени, в связи с чем в период лечения рекомендуется мониторинг картины крови и уровня печеночных ферментов, однако эти побочные эффекты встречаются значительно реже, чем при применении других нормотимиков (табл. 3).
Ламотриджин не оказывает существенного влияния на лабораторные показатели, не вызывает метаболических побочных эффектов, прибавку массы тела и инверсию фазы у больных БАР [9, 35, 36, 40, 41]. При длительном применении он не влияет на прогрессирование атеросклеротического процесса [42] и имеет более благоприятный нейрокогнитивный профиль по сравнению с другими антиконвульсантами [43].
В отличие от карбамазепина и вальпроата ламотриджин не только не ухудшает сексуальные функции, а возможно, и улучшает их [44].
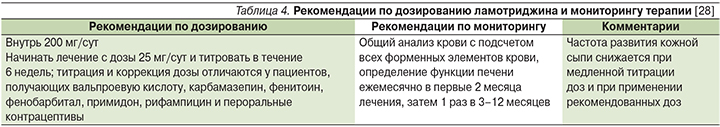
Наибольшее беспокойство при применении ламотриджина вызывает риск развития синдрома Стивенса–Джонсона и токсического эпидермального некролиза. Повышение частоты развития этих осложнений в 3 раза по сравнению с группой плацебо было выявлено в первых клинических исследованиях препарата на пациентах с эпилепсией при применении в более высокой, чем рекомендуется в настоящее время, стартовой дозы, быстрой титрации доз и при одновременном применении вальпроата [9]. Риск развития серьезной сыпи составил 0,3% у взрослых и около 1% у детей [45]. Однако впоследствии было показано, что при правильном режиме подбора дозы эти реакции развиваются редко [32]. Частота развития серьезной сыпи у пациентов с БАР во всех клинических исследованиях составила 0,1%, в т.ч. 0,08% у пациентов, получавших ламотриджин в виде монотерапии, и 0,13% – у пациентов, получавших его в качестве адъювантного препарата [46]. Согласно мета-анализу 21 проспективного постмаркетингового исследования, риск развития сыпи при правильном применении ламотриджина (табл. 4), достоверно не отличается от такового при применении других противосудорожных препаратов, лития и плацебо [47].
Существенным преимуществом ламотриджина перед традиционными антиконвульсантами является отсутствие у него выраженного отрицательного влияния на когнитивные и поведенческие функции [48]. Он редко ассоциируется с когнитивным дефицитом [49, 50], а при его применении в качестве дополнительной терапии при эпилепсии наблюдается улучшение когнитивных проблем [48]. У взрослых и детей с БАР применение ламотриджина ассоциировалось с улучшением памяти [43, 51].
Ламотриджин хорошо сочетается с большинством психотропных препаратов [13]. Осторожность следует соблюдать лишь при одновременном применении вальпроата, угнетающего метаболизм ламотриджина, и карбамазепина, индуцирующего его клиренс.
Отличная переносимость ламотриджина способствует повышению приверженности пациентов лечению, что является важной проблемой для пациентов с БАР, более половины из которых не могут аккуратно соблюдать назначения врача в течение года [52]. Важным для больных БАР является отсутствие у ламотриджина (в отличие от вальпроата и атипичных антипсихотиков) метаболических побочных эффектов и негативного влияния на массу тела, поскольку у них повышен риск развития ожирения, сахарного диабета 2 типа и сердечно-сосудистых заболеваний [53, 56].
Благоприятный профиль безопасности, редкая частота побочных эффектов и отсутствие отрицательного влияния на настроение, когнитивные функции способствуют повышению качества жизни пациентов, что является одной из целей лечения БАР [57]. Эти свойства также обусловливают преимущества ламотриджина для лиц пожилого и старческого возраста, в т.ч. с деменцией [58], и у детей [59]. Есть данные, согласно которым пожилые пациенты даже лучше, чем молодые, переносят ламотриджин, в частности, у них ниже риск развития кожных сыпей [60].
Ламотриджин имеет существенные преимущества перед вальпроатом у женщин детородного возраста [61, 62]. Он представляется самым безопасным антиконвульсантом во время беременности [63]. В анализах регистров беременности и других исследований большие врожденные аномалии наблюдались у 0–3,2% детей (по сравнению с 6,2–16,0% при применении вальпроата), внутриутробно подвергшихся действию этого препарата, что не отличается от частоты врожденных аномалий у населения в целом [64–67].
В нескольких исследованиях показано небольшое повышение риска развития ротолицевых расщелин под его влиянием, однако оно не подтвердилось в недавно опубликованном анализе 21 регистра беременности (10,1 млн рождений в период с 1995 по 2011 г.) [67]. Акушерских или неонатальных осложнений, связанных с применением во время беременности монотерапии ламотриджином, не описано. В отличие от вальпроата он не ассоциировался с нейроповеденческой токсичностью у детей, внутриутробно подвергшихся его воздействию [68].
Таким образом, ламотриджин является эффективным препаратом для лечения БАР с преобладающей антидепрессивной активностью. Он эффективен при остром эпизоде депрессии, но наиболее большое значение имеет для длительной поддерживающей терапии пациентов с преобладающей депрессивной симптоматикой. Преимуществом ламотриджина перед другими нормотимиками, особенно при длительном применении, является его высокая безопасность, в т.ч. в отношении детей, лиц пожилого возраста и беременных женщин.



